
Personalized cultural journeys for post-surgical recovery.
Evidence-based mobilization delivered through cultural engagement in the surgical ward.
Post-Surgical Inactivity Costs Lives and Hospital Resources
Motivational interviewing improves postoperative mobilization in ERAS colorectal surgery
Early postoperative mobilization is feasible after colorectal surgery
Physical activity after major abdominal cancer surgery is far from optimal
Wearable activity monitors correlate with length of stay after major surgery
Mobilization reduces composite postoperative complications after major surgery
Early postoperative mobilization is feasible after colorectal surgery
Wireless technology assesses mobility recovery in elderly patients after major surgery
Mobilization reduces composite postoperative complications after major surgery
Physical activity after major abdominal cancer surgery is far from optimal
Activity tracking after surgery correlates with postoperative complications
Complication Risk
Immobility after surgery increases risk of thromboembolism, atelectasis, pneumonia, muscle atrophy, and extended hospital stays.
Physical activity after major abdominal cancer surgery is far from optimal
Mobilization reduces composite postoperative complications after major surgery
Early postoperative mobilization is feasible after colorectal surgery
Activity tracking after surgery correlates with postoperative complications
Prolonged Recovery
Patients struggle to mobilize, leading to slower healing and delayed discharge readiness.
In-hospital mobilization impacts physical functioning after lung cancer surgery
Physical activity declines after gastrointestinal or bladder cancer surgery
DOI: 10.1111/ecc.13739
Fear & Anxiety
Pain, fear of falling, equipment tethering, and unstimulating hospital environments keep patients immobile when they need to move.
Systematic review of barriers to physical activity in hospitalized older patients
Barriers and facilitators to mobility in hospitalized patients: systematic review
Nurse Capacity
Peak morning care cycles leave little time for mobilization support in busy surgical wards.
Staff shortages as barrier to patient mobility in hospitals: qualitative study
Barriers and facilitators to mobility in hospitalized patients: systematic review
Safe Mobilization Meets
Cultural Engagement
Culture Care transforms post-surgical corridors into personalized recovery paths. Patients move safely at their own pace, guided by familiar music and brief cultural moments, while clinical outcomes improve without adding nurse burden.
Simple 5-minute setup for personalized recovery experience
Four Pillars of Effective Mobilization
Rooted in behavioral science and clinical safety, these pillars make walking easier, safer, and more meaningful for post‑surgical patients.
Motivation
Familiar music increases willingness to walk and reduces perceived effort, helping patients exceed minimum mobilization targets.
Autonomy
Adaptive routes match individual capacity using previous session data, enabling patients to walk independently when safe and with support when needed. Duration adapts to each patient's daily condition—from 5 to 60 minutes.
Safety
Bone‑conduction audio keeps alarms audible. Rest zones and call buttons are embedded along the path with clear wayfinding.
Personalization
Era, listening style (music-first vs light voice), and duration are tailored to each patient—turning corridors into meaningful recovery paths.
Quick Setup in 5-10 Minutes
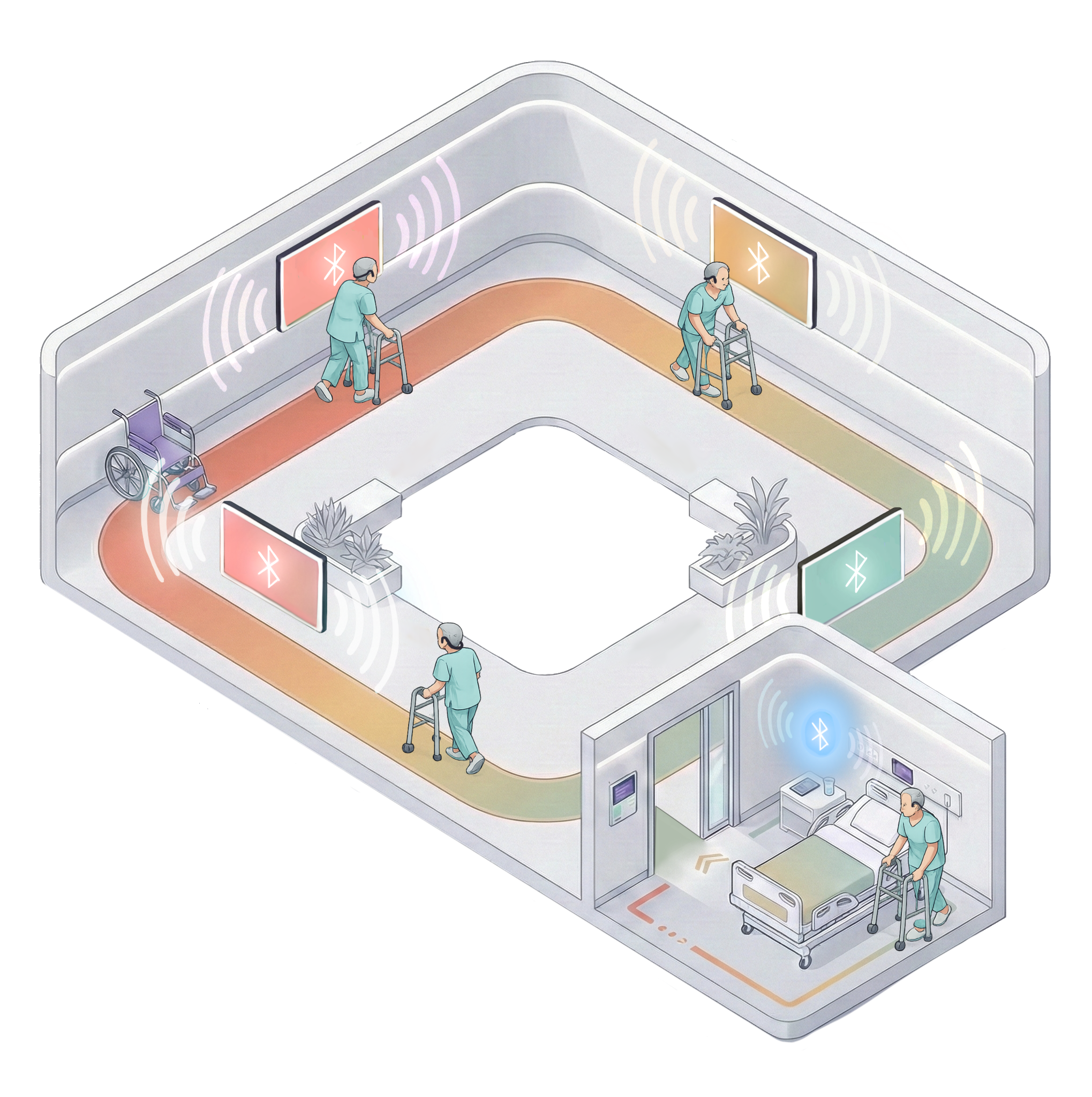
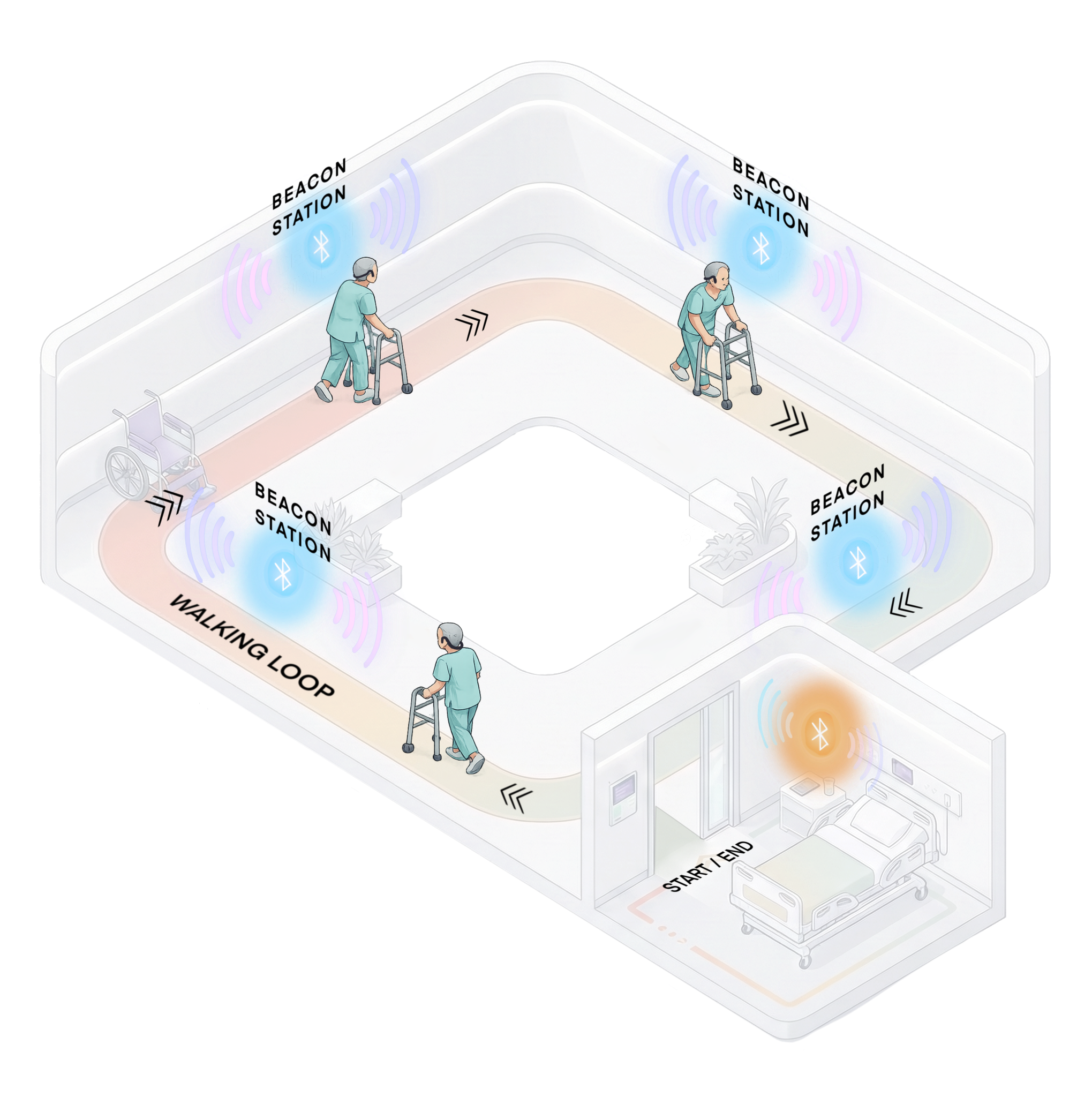
The Complete Patient Journey
From initial setup in the patient room to autonomous walking through beacon-enabled corridors and back—this visualization shows how Culture Care transforms post-surgical recovery. Patients move at their own pace, guided by personalized cultural audio that activates automatically at each station, while clinical data is captured seamlessly in the background.

Preparation
Patient receives wearable device with simple controls and headphones
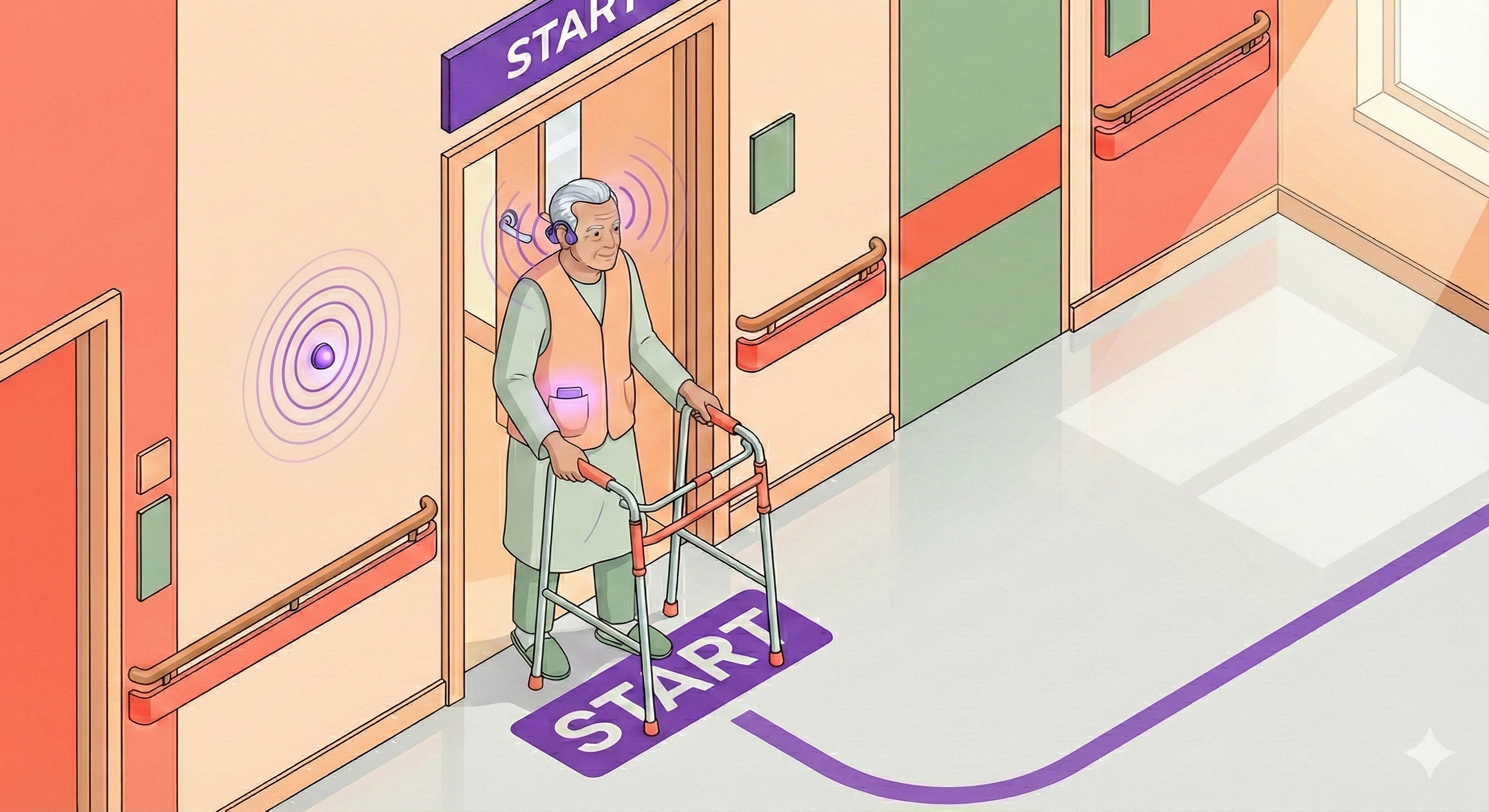
Journey Start
Walking begins, first beacon detected, the sound world begins (calming regulation layer)

Station Progress
Patient moves through multiple beacons, audio adapts to walking pace
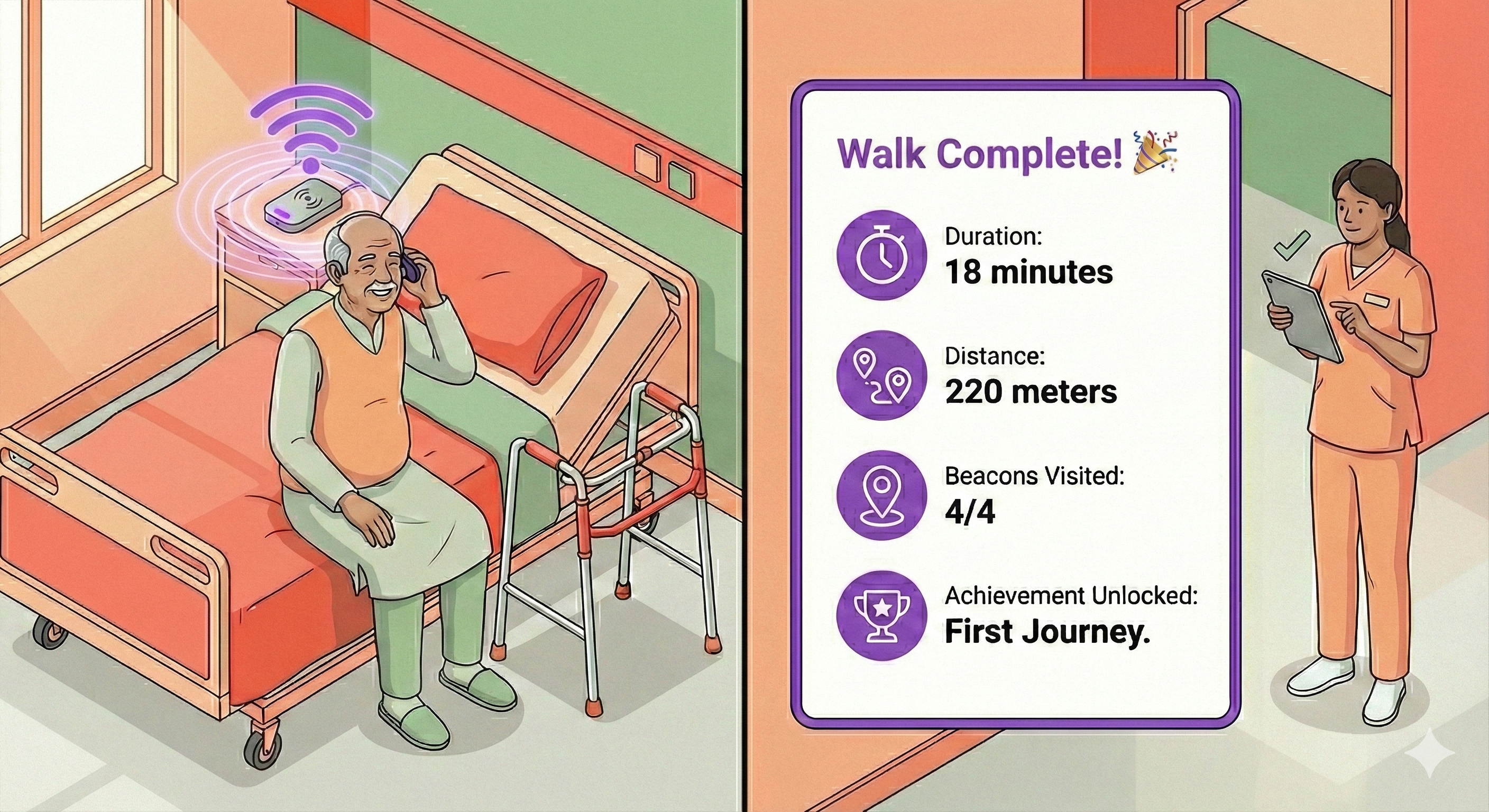
Completion
Session ends with meaning-first closure; clinicians can review trends; patient metrics are optional
Instant Patient Opt-In
Flyers and a QR code are provided at admission or bedside so patients can enroll instantly. No staff coordination required—patients self-register and choose their preferences independently.
5-Minute Assessment
Nurse quickly evaluates mobility level, pain, and cognitive status to determine appropriate assistance level. Designed to fit existing care rhythms with minimal additional workload.
Personalized Content
Familiar cultural audio reduces anxiety and provides natural pacing for safer gait. Patients choose their era and listening style through a simple touch interface—no training needed.
Adaptive Route
Routes adjust daily based on each patient's capacity—using mobility data, pain levels, and fatigue from previous sessions. Accommodates medical equipment like mobile O₂, drains, and walking aids.
Safety Built-In
Bone-conduction audio preserves alarm audibility. Rest zones every 15-20m with visual markers and call buttons. UV hygiene protocols enable safe equipment reuse. Patients are matched to appropriate assistance levels based on their cognitive, cardiorespiratory, and functional status.
Continuous Monitoring
Step count, session duration, and engagement patterns are captured automatically via IMU sensors. Clinicians can review mobility trends without additional charting burden; patient-facing data can be offered as an optional tab (no targets, no pressure by default).
Built for Real-World Deployment
Crank Studio’s Digital Twin validates beacon placement, RSSI thresholds, and end-to-end patient flow before installing hardware in the hospital.
Why Simulation Matters
-
Test beacon placement before physical installation—identify dead zones, optimize trigger distances, validate floor plan layouts
-
Calibrate RSSI thresholds with real-time signal strength values that match what the ESP32 reports
-
Validate end-to-end flow (CAT 1/2/3) and demo the system without needing a corridor install
Hardware Validation Platform
We used Crank Studio’s Digital Twin to validate the beacon-triggered experience before deployment.
Request Demo AccessA Layered Sound World (Regulation + Discovery)
A living, reassuring sound world where people collect small moments over time—not a story they must follow. Between stations: regulation (bed, minimal voice). At stations: discovery (short, complete “windows”).
Beacon-Triggered Moments (“Open Windows”)
A gentle bed plays continuously while patients walk (regulation); brief “window” moments appear at stations (discovery)
Small Moments
Between stations is primarily regulation (stable bed, low cognitive load). At stations, a short, complete moment plays—something you can collect without needing to “keep up” with a storyline.
Gentle voice (not pressure)
Voice is used sparingly and predictably. Continuity is carried by motif and tone—not cliffhangers—so stopping early still feels complete.
Cultural Resonance
Culturally diverse stories and gentle soundscapes selected to create meaningful connections without overwhelming the walking experience. Audio supports movement, not the other way around.
Potential Benefits of Culture Care
Expected impacts of cultural engagement on post-surgical mobilization and wellbeing—currently under rigorous evaluation at Neuchâtel Hospital
Mobilization
- Increased daily step count
- Longer walking periods
- Decreased daily time spent lying in bed and increased daily time spent in upright position (which is already great in a respiratory and hemodynamic point of view)
- More even distribution of physical activity throughout the day (not only morning or afternoon)
- Higher proportion of patients achieving mobility recommendations from the Enhanced Recovery After Surgery (ERAS) Society
Patient Experience
- Better mood through familiar cultural content and personalized experiences
- Reduced fear and anxiety around mobilization
- Distraction from feelings of fatigue during exercise
- Meaningful connection to cultural heritage during recovery
Safety by Design
Zero added complications through careful protocol design. Rest zones every 15-20m with brief, bounded audio moments (optional), call button protocols for patient safety, and bone-conduction audio to preserve medical alarm audibility.
Nurse Workload
Designed for zero added workload for nursing staff. ~5-minute CAT categorization fits care rhythms, CAT 1 patients require no supervision, and UV hygiene box enables autonomous equipment reuse.
Rigorous Clinical Evaluation
Mixed quantitative and qualitative study approved by CER-VD (Cantonal Ethics Committee for Research on Human Beings) in March 2025
ClinicalTrials.gov identifier: NCT06893848
Quantitative mobility data (IMU sensors, beacon tracking) + qualitative interviews with patients and nursing staff conducted by Haute École Arc Santé
On-site pilot: March 2026 | Quantitative phase: 2026–2027 | Qualitative phase completion: Sept 2028
Built for hospitals. Safety by design
Safety mechanisms are embedded by design, and the protocol is under ethics-approved clinical evaluation.
Built for Hospitals
Pre-deployment evaluation of hospital layout and patient flow
Coordinated session planning integrated with ward routines
Medical device compatibility and charging infrastructure
Comprehensive onboarding for clinical teams and escorts
Safety by Design
Keeps medical alarms audible
Clear visual markers throughout route
Placed along route for assistance
Equipment turnaround sterilization
Venous or urinary catheter, drain transport, oxygen adaptation
Falls risk patients require escort
Recognition & Media Attention
Our team's work on culture-as-therapy—including museum prescription programs—has captured international attention, validating the therapeutic power of cultural engagement in healthcare.
Building on proven concepts: Cultural prescriptions have shown that arts and cultural interventions can be integrated into healthcare. Culture Care advances this idea by embedding personalized cultural experiences directly in the recovery environment—where patients need them most.
Supported By
We're grateful for the generous support of these organizations who believe in the power of culture to transform healthcare.









Who's Behind Culture Care
A multidisciplinary team bringing together clinical expertise, innovation, research, and design.
Prof. Dr. Marc-Olivier Sauvain
President & Project Leader
Head of Surgery Department, Neuchâtel Hospital Network (RHNe)
Vice President of the Swiss Society of Surgery. Leading the implementation and serving as co-researcher on the clinical pilot study.
Dr. Jonathan Dugernier
Treasurer & Principal Investigator
Associate Professor, Haute Ecole Arc Santé · Physical Therapist, RHNe
Physiotherapist, expert in the respiratory field, with experience at Cliniques universitaires Saint-Luc (Brussels, Belgium) and Neuchâtel Hospital (Switzerland), working in the intensive care unit, the emergency department, and general wards. Jonathan is an associate professor at Haute Ecole Arc Santé, Physiotherapy, involved in research, including the Culture Care project.
Dr. Stefano Maddalena
Secretary
Director, Innovation Laboratory · Audemars Piguet
Bringing design thinking and innovation methodology to transform the hospital environment.
Allison Crank
Experience Design x Technical Lead
Founder & Director · Crank Studio — Design & Technology
Leading the end-to-end experience design and technical development of Culture Care—from patient experience, spatial and audio design to system architecture and implementation.
Mathieu Jaton
Cultural Partnership Director
Director, Montreux Jazz Festival
Swiss cultural manager and director of the iconic Montreux Jazz Festival. Bringing decades of expertise in cultural programming and audience engagement to shape the musical content strategy and ensure authentic cultural experiences for patients.
Olivia Lohmeyer
Psychological Research & Human-Centered AI
Leading applied psychological research informing the scientifically grounded development and implementation of the patient experience—integrating behavioral science, motivation research, and human-centered AI frameworks.
Research & Implementation Partners
Partner With Us
We're seeking hospital partners, clinical collaborators, and funding to scale evidence-based post-surgical mobilization beyond Neuchâtel.
Hospital Partners
Surgical departments ready to pilot CAT-adapted mobilization with co-development of protocols and outcome data sharing.
Clinical Collaborators
Surgical teams, physiotherapists, nursing researchers, and medical device advisors.
Investment Partners
Seed funding for multi-site expansion, hospital deployment, and clinical validation studies.
Get in Touch
Ready to collaborate? Fill out the form and we'll connect you with the right team member.





